
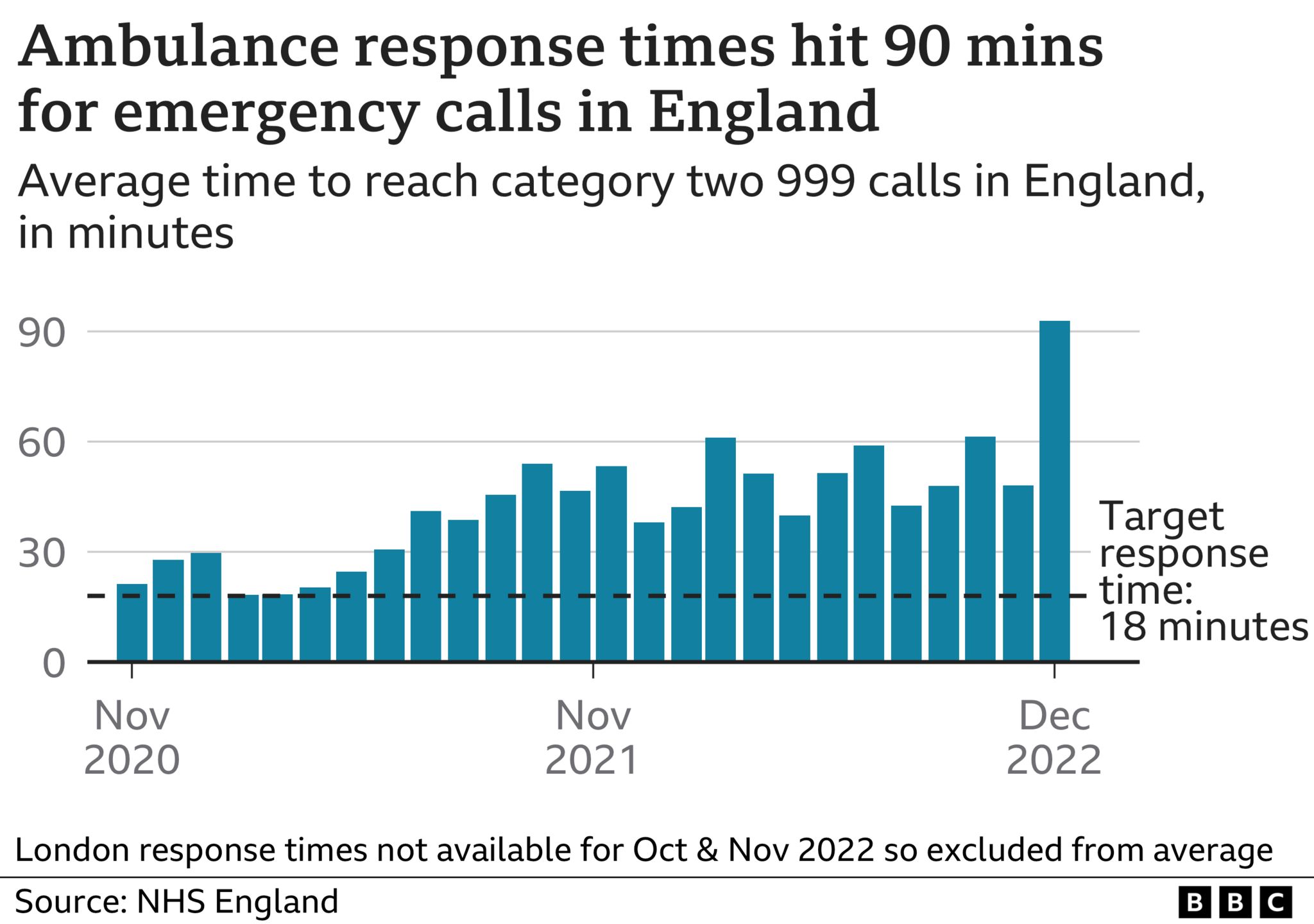
Patients with emergencies such as heart attacks and strokes in England had to wait more than 90 minutes on average for an ambulance at the end of 2022.
It came after a sharp deterioration in 999 response times in December – they were nearly twice as bad as November.
Record worst waits were also recorded for life-threatening cardiac arrests, while A&E waits of over four-hours reached their highest level ever.
Patient groups warned the delays would be leading to real harm.
Combined, the data – released by NHS England – represents the worst-ever set of emergency care figures since modern records began in 2004.
The figures show:
- Average waits of more than 90 minutes to reach emergency calls such as heart attacks – five times longer than the target time – with waits of over 150 minutes in some regions
- Response times for the highest priority calls, such as cardiac arrests, taking close to 11 minutes – four minutes longer than they should
- More than a third of patients in A&E waiting longer than four hours
- One in seven patients waiting more than 12 hours for a bed on a ward when they need to be admitted
- But there has been some progress with the waiting list for routine treatment falling slightly, to 7.19m by the end of November
“Pressures on the NHS right now are intolerable – with patients paying the price,” said Louise Ansari, national director of the Healthwatch England patient group.
The Royal College of Emergency Medicine believes up to 500 people a week could be dying because of the problems accessing emergency care.

‘My dying husband could not get an ambulance’
This video can not be played
To play this video you need to enable JavaScript in your browser.
When Martin Clark, 68, started suffering with chest pains at home in East Sussex in November, his wife immediately called an ambulance.
But none came. She phoned another three times before her and her son decided to drive Martin to hospital themselves 45 minutes later.
When they arrived, the father-of-five went into cardiac arrest and, despite receiving medical attention, died.
His wife, Ann, said while waiting for an ambulance Martin had been crying out in pain and at one point wrote a note saying: “I don’t think I’m going to make it. Love you.”
It was excruciating, she said, adding: “He was let down very badly. They should have come.”
The case happened before any strike action was held in the NHS.
The South East Ambulance Service has apologised for not being able to send a crew.

Downing Street said “people will be rightly concerned” by the waiting time figures.
The prime minister’s spokesman added the ambulance waits in particular were clearly “not acceptable” and tackling the problems was one of the government’s key priorities.
The Healthcare Safety Investigations Branch, which investigates incidents in the NHS, has previously warned about the risk to patients from ambulance delays.
One of the key problems is the long delays crews face at accident and emergency units.
The handover of patients should be done within 15 minutes – but in November, a third of handovers took more than 30 minutes.
By the end of the December, this had risen to more than 40%.
Unions say patient safety is one of the key reasons ambulance staff are striking. Wednesday saw the second walkout of the winter by crews in England and Wales.
‘Extreme delays can’t be new normal’
Dr Sonya Babu-Narayan, of the British Heart Foundation (BHF), said “The difference between life and death can be a matter of minutes when someone is having a heart attack or stroke.
“Extreme delays to emergency heart and stroke care cannot become a new normal.
“Healthcare staff are doing all they can – but there aren’t enough of them and many will be working in difficult conditions without fit-for-purpose facilities.”
The Department of Health and Social Care said it recognised the pressures the NHS was facing following the pandemic and was “working tirelessly” to ensure people received the care they needed.
This included an extra £750m being invested this winter to free up hospital beds and unlock some of the delays in the emergency-care system.
This is being targeted at improving care in the community as one in eight hospital beds are occupied by patients who are medically fit to leave but cannot be discharged because they need support.

Have you been affected by the issues raised in this story? Share your experiences by emailing haveyoursay@bbc.co.uk.
Please include a contact number if you are willing to speak to a BBC journalist. You can also get in touch in the following ways:
- WhatsApp: +44 7756 165803
- Tweet: @BBC_HaveYourSay
- Upload pictures or video
- Please read our terms & conditions and privacy policy
If you are reading this page and can’t see the form you will need to visit the mobile version of the BBC website to submit your question or comment or you can email us at HaveYourSay@bbc.co.uk. Please include your name, age and location with any submission.

