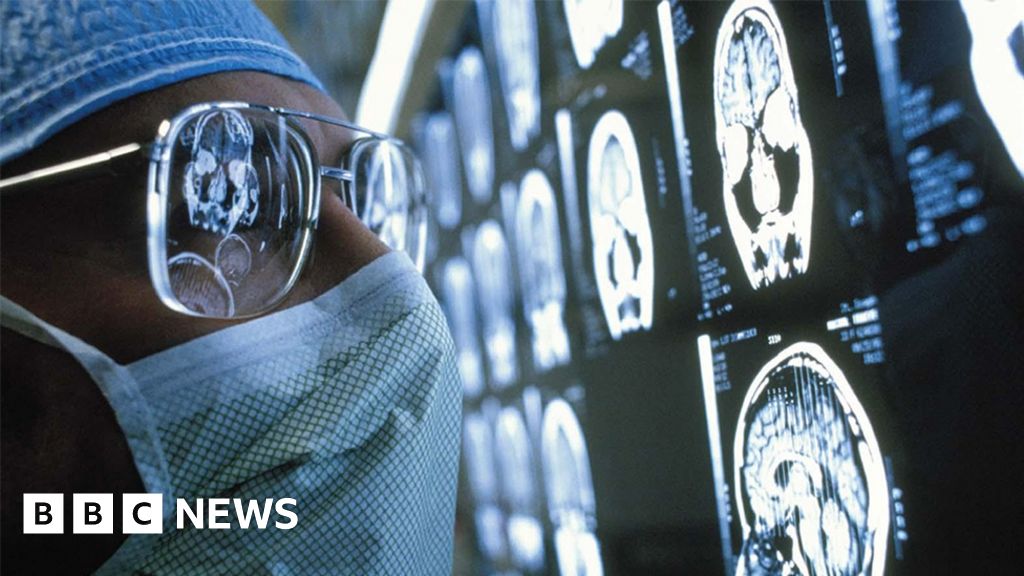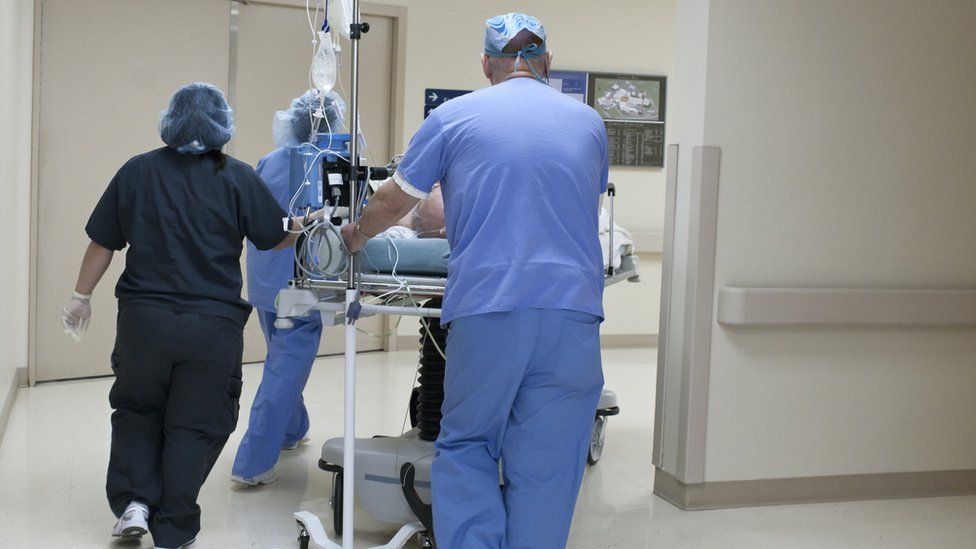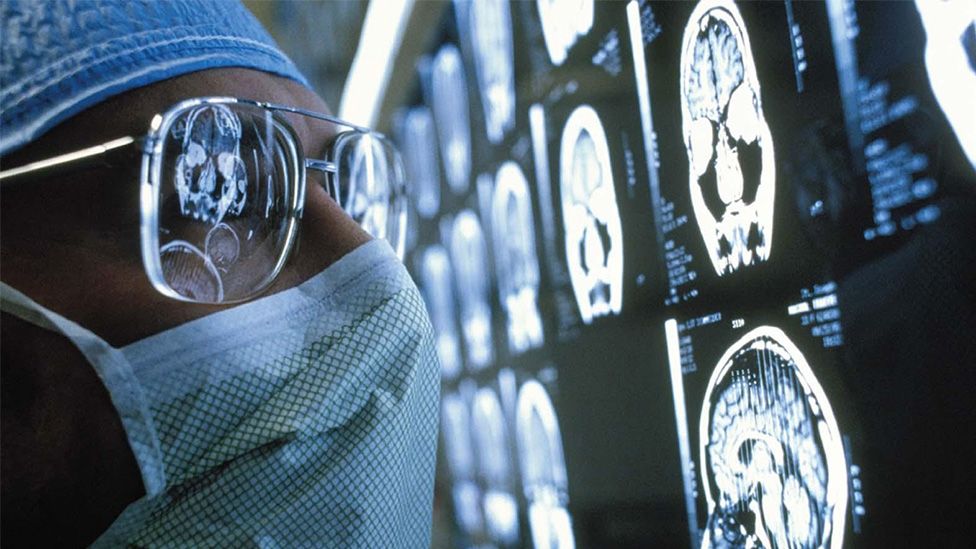
The NHS is struggling to provide safe and effective care for all cancer patients, say senior doctors.
The Royal College of Radiologists is warning that all four UK nations are facing “chronic staff shortages”, with patients waiting too long for vital tests and treatments.
Half of all cancer units are now reporting frequent delays for both radiotherapy and chemotherapy.
Ministers say a workforce strategy for the NHS in England is due shortly.
The plan, which is meant to spell out how the government will plug staffing gaps over the next 15 years, has been repeatedly delayed, to the frustration of some in the health service.
In other parts of the UK, ministers say cancer waiting lists are a priority and extra investment is being made in staff and diagnostic equipment.

In June 2022, Carol Fletcher, from South Wales, finally had her routine screening appointment for breast cancer, which was itself overdue.
“It took another eight weeks after my mammogram before I was told there might be something wrong,” she said.
Since her cancer diagnosis, there have been more waits – for scans, tests, surgery and then chemo.
“I was told that I might not get results back [quickly] after my mastectomy because they haven’t got enough pathologists, so there was another eight-week delay for chemotherapy,” she said.
“I can’t plan for the future and it’s had a huge impact on my family.”

NHS services across the whole UK have been struggling to meet cancer targets since well before Covid.
The pandemic increased the backlog, with scans and treatment disrupted by lockdowns.
Across England, Scotland and Northern Ireland, one key target is to start treatment within two months of an urgent referral by a GP.
In Wales the measure is slightly different as it includes all urgent and non-urgent referrals.
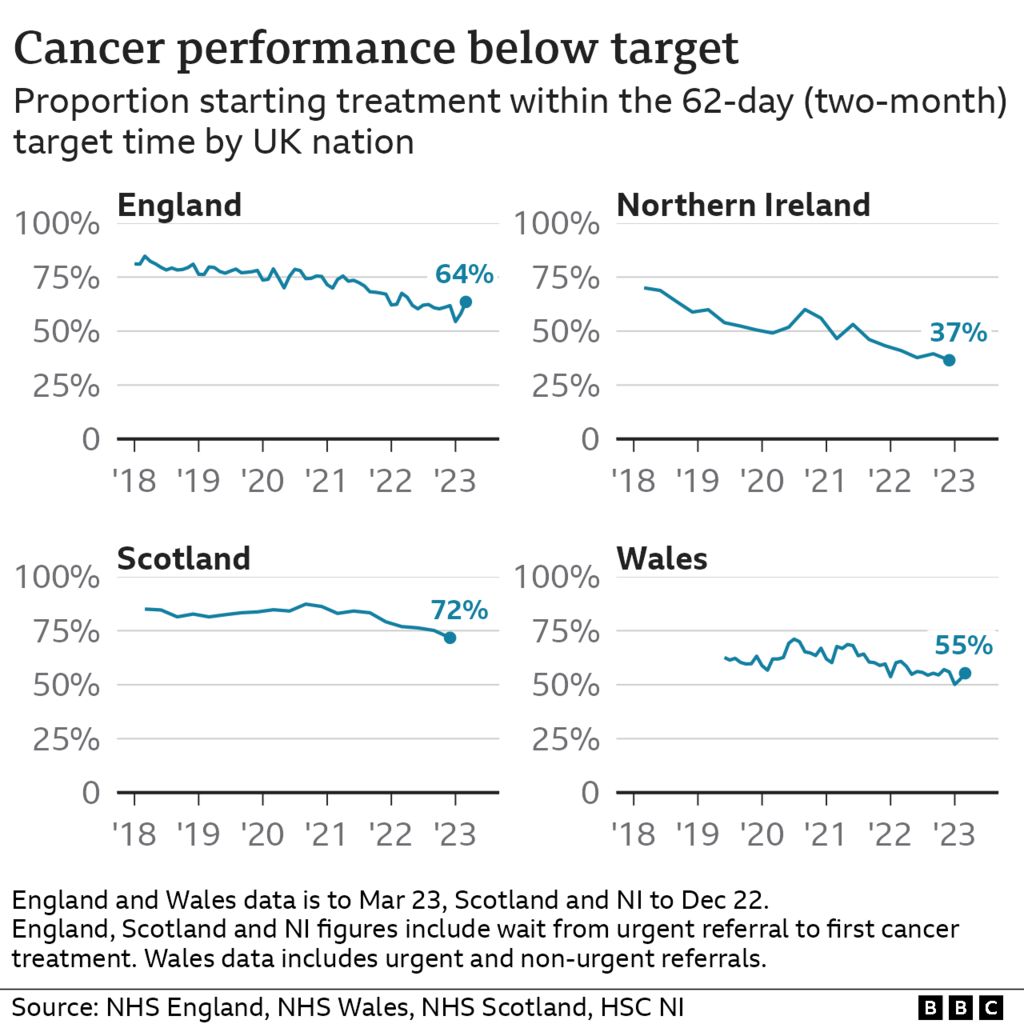
All four nations are operating well below those levels. In England just 64% of patients start treatment in that time against a target of 85%.
Growing delays are, in part, the flip side of a medical success story.
Scientific progress in cancer care has been remarkable, with cutting-edge drugs offering hope where previously there was little that could be done.
New techniques are more effective but often far more complex for doctors to deliver.
At the same time the UK population is getting older – and as cancer risk is strongly linked to age it means more more demand for expensive scanners, along with more staff to analyse those scans, and more specialist doctors and nurses.
The Royal College of Radiologists (RCR) describes the situation as a perfect storm – and says the workforce is struggling to keep up.
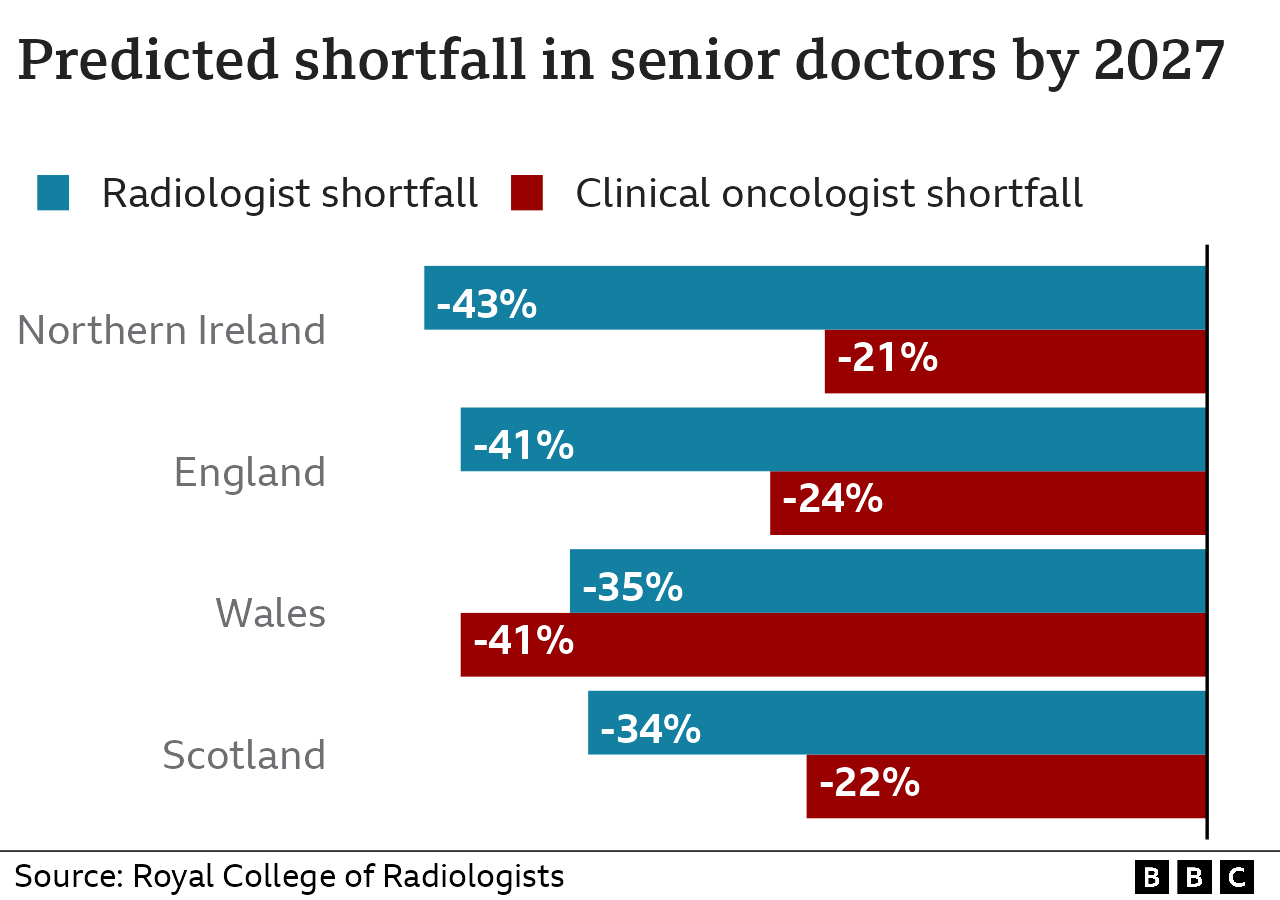
Across the four UK nations, it calculates there is now a 15% shortfall of specialist cancer doctors – or clinical oncologists – who deliver chemotherapy and radiotherapy.
Without action, it says this gap will grow to 25% – or a shortage of 368 full-time consultants – by 2027.
Just as concerning is an even larger shortage of consultant radiologists – highly trained doctors who interpret scans to diagnose cancer or monitor its progression.
‘Perfect storm’
The RCR says for each month a patient waits to start cancer treatment, the risk of death is increased by about 10%.
In its annual survey, 44% of cancer service managers say they are now “highly concerned” about patient delays, up from 29% in the previous year.
“There are examples in almost every cancer centre where parts of the service just aren’t running as well as we would like,” said Dr Tom Roques, a consultant oncologist and vice-president of the RCR.
“We’re having to tell patients all the time that we can’t quite treat them as quickly as we would like, or in the way that we’d like, and that’s a stressful thing to have to do.”

Kevin O’Hara, 60, from County Durham, broke five ribs in a motorbike accident last November.
A scan of his upper body also picked up a shadow near one of his kidneys that was later diagnosed as cancer.
He was offered drug treatment meant to slow the growth of the tumour and – in early February – was told the waiting list for surgery would be three to four months.
That period has now been and gone but he is still waiting for a date for his operation.
“Every day you are waiting and waiting and nothing changes,” he said.
“I come home from work and go to the door and, when there’s no envelope that says NHS on the top, I just get so depressed.”
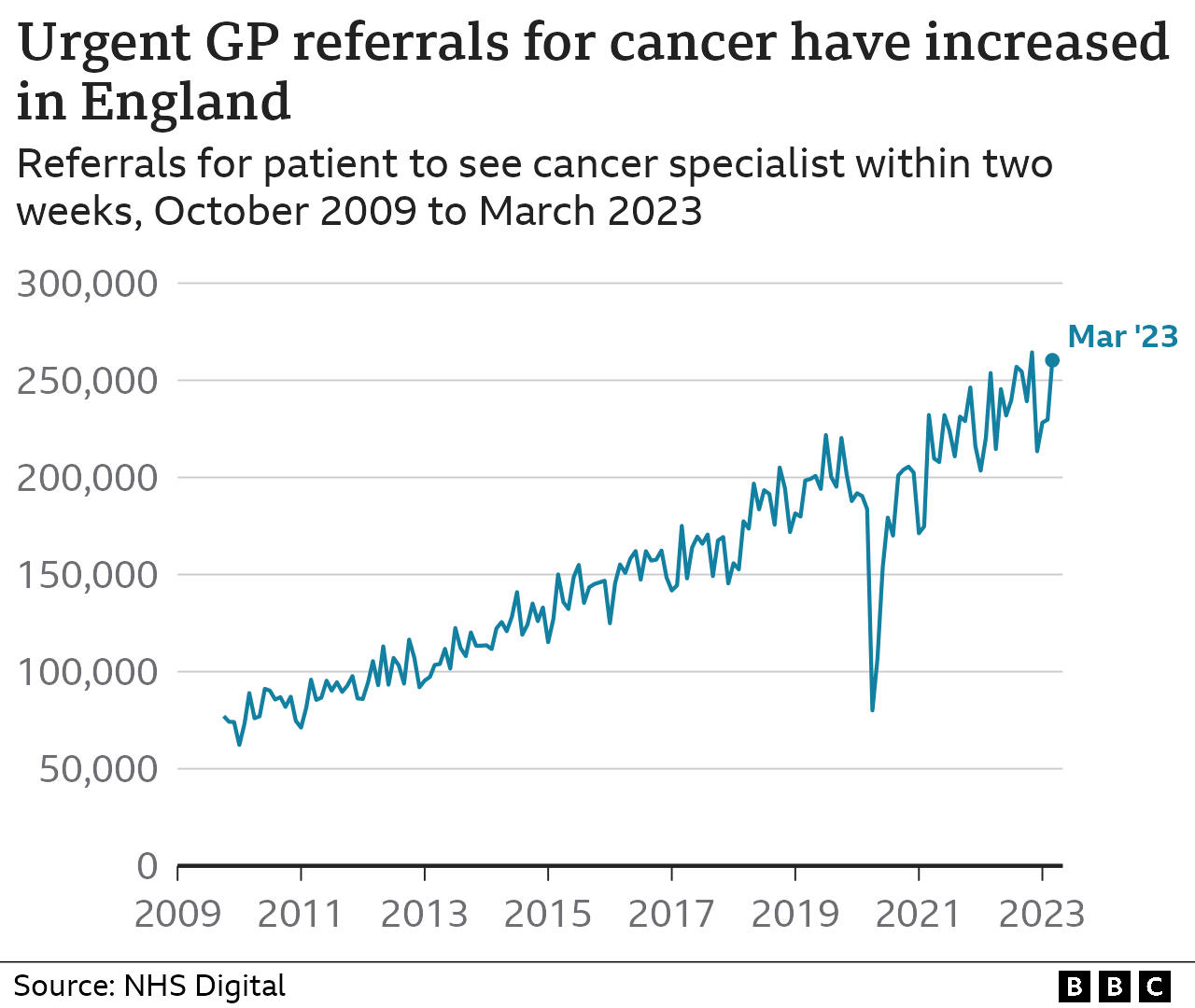
There is another trend in cancer care which is often overlooked.
The last decade has seen a dramatic increase in people coming forward to get checked after spotting a possible symptom such as an unusual lump, strange mole or unexplained weight loss.
The reasons for that are complex and include a bounceback in demand since Covid, stronger guidance for GPs to refer to cancer specialists, major NHS publicity drives and the work of campaigners such as “Bowelbabe” Deborah James.
Cancer doctors view the spike in demand as a “very good thing”, as a growing proportion of patients are now diagnosed earlier when cancer is easier to treat.
But it also puts more pressure on NHS services, with waiting times for diagnosis and other scans one of the key bottlenecks in the system.
Since Christmas there have been some signs of progress, with the NHS in England reducing the backlog of long waits for treatment and hitting one of its other standards – for faster diagnosis – for the first time.
This video can not be played
To play this video you need to enable JavaScript in your browser.
The RCR also says there is a “chink of light” – with recruitment of oncologists rising over the last three years, particularly in parts of the country with the worst staff shortages.
It wants each UK nation to increase medical school places and training posts, and says more also needs to be done to stop experienced staff cutting their hours or leaving the profession early.
The Department of Health said that the total number of full-time staff in the cancer workforce in England had risen by 51% to 33,093 since 2010.
A spokesman added: “We want to build on this progress and will publish a workforce plan shortly to ensure we have the right numbers of staff, with the right number of skills.”
The Scottish government is also expected to publish its new 10-year cancer strategy within weeks, setting out ways to attract and retain more staff.
The Welsh government recently published a cancer improvement plan and says it is now investing heavily to train more staff and build more diagnostic and treatment centres.
In Northern Ireland, the health department said it is “extremely disappointing” that cancer targets are being missed. It has recently opened two new rapid diagnostic centres and started a “cancer strategy workforce review”.
Data visualisation by Liana Bravo.
Follow Jim on Twitter.
Related Topics
-
-
6 days ago
-